One of the signature efforts of the current administration was to de-fund research into healthcare disparities as part of their “anti-DEI” policy. This was done despite the enormous scope of the problem in the US. For example, Black women are far more likely than white women to die in the peripartum period even when accounting for differences in income and education level. We can’t tackle problems like this without knowing more about them, and cutting off funding means more people will suffer and die.
A recent study highlights ways in which research into health disparities saves lives. Until very recently, kidney function on lab reports had two numbers—one to use if the patient was African American, and another if they were not. This was based on a false assumption that Black people’s kidneys work better than the lab results would indicate. This assumption was never based on good science. And if you think this was some remnant of early 20th century medicine, you’d be wrong—reporting kidney function by race came about at the beginning of the 21st century. The use of these race-based equations falsely labelled African American patients as having better kidney function than they actually did and led to delays in life-saving care such as kidney transplantation.
A few years ago we finally got rid of the erroneous kidney measurements we were using for Black people, but these patients were still waiting longer than others for transplants. So the Organ Procurement and Transplantation Network started a policy of re-listing patients who were lower on the transplant list due to these false, race-based equations. A research group at Harvard wondered what effect this new policy had.
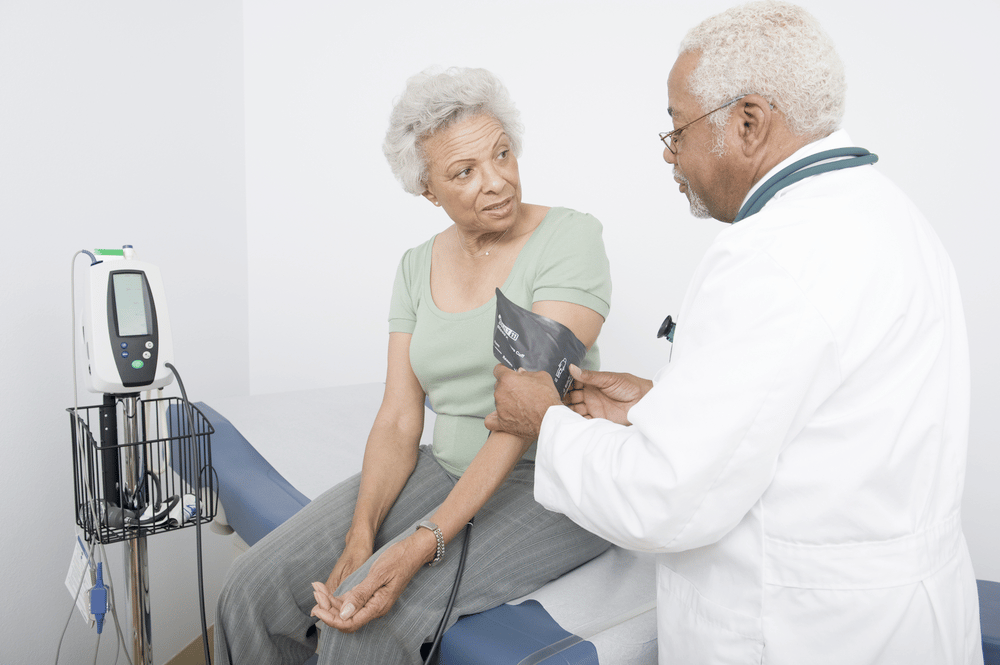
Kidney failure affects African Americans at 3-4 times the rate of white people (From National Institutes of Health)
What they found was very encouraging—kidney transplant rates for Black patients increased significantly. Some might call a corrective policy like this “DEI” or “affirmative action”, policies abhorrent to our current administration. One of the arguments they make is that it’s unfair to correct past inequities because it will come at the expense of others. In this study, we didn’t see that at all. Improving transplant access for Black patients did not reduce transplants in non-Black patients. It simply helped people who had been wrongly denied life-saving care.
Rooting out racist assumptions in medicine isn’t a game. It isn’t some lefty, ideological plan to keep white people down. It is how we improve the health of ourselves and our neighbors. It turns out that healthcare isn’t a zero-sum game. This study showed that eliminating racist practices doesn’t benefit one group at the expense of another—it helps all of us. We have plenty of resources, we just distribute them inequitably. Choking off funds to fix these problems doesn’t help anyone—it makes us all less healthy and less moral.